Prediabetes (Insulin-Resistance)
Prediabetes/Insulin-Resistance
In normal metabolism, insulin is secreted from the beta cells of the pancreas in response to carbohydrates in the diet. One of the functions of insulin is allowing carbohydrates to have access to the mitochondria of cells where they are converted into fuel (ATP) that is used by cells to perform their normal functions.
Sometimes, however, that process doesn’t occur as efficiency as it was designed. Cells do not respond appropriately to the carbohydrate signal and excess insulin is required to allow them to enter the cells.
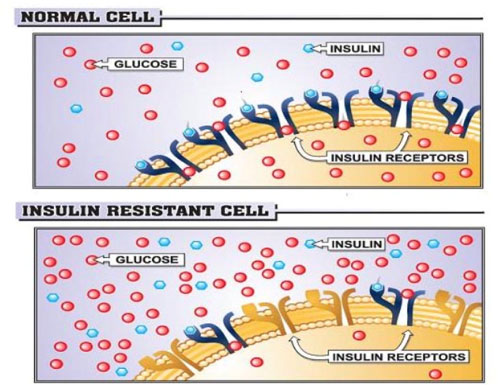
There are many reasons this dysfunction occurs. For example, normally insulin will link to a receptor on the surface of the cell to begin the process that allows carbohydrates to enter cells. If there is a lack of receptors, insulin will be inefficient in allowing cells to produce energy and all their functions will be impaired.
Figure 1 depicts the decrease number of insulin receptors in normal cells and insulin-resistant cells.
Since insulin is a fat-storing hormone, more fat will be stored, especially in the abdomen.
Many abnormal chemical reactions can occur at the site where insulin links to its receptor. Again, this will impede the ability of insulin to allow carbohydrates to enter cells. The pancreas will produce excess insulin in an attempt to force carbohydrates into cells, something that will lead to more fat deposits.
Certain proteins and/or enzymes released by the stored fat act on muscle and liver cells to impair the way they “read” insulin signals to process glucose appropriately. There also genetic factors that could disrupt the insulin/glucose interaction, causing it not to function properly. And, lifestyle and diet play a major role for this process to function in an optimal manner.
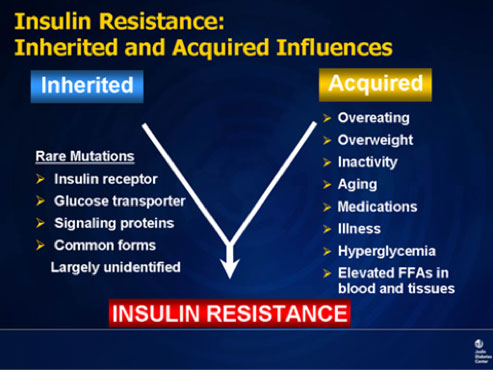
Look at Figure 2.
You have the option to make the proper lifestyle choices to control overeating, being overweight and inactivity.
The health consequences of excess insulin (insulin resistance) are overwhelming. They can shorten your life and markedly impair the quality of it.
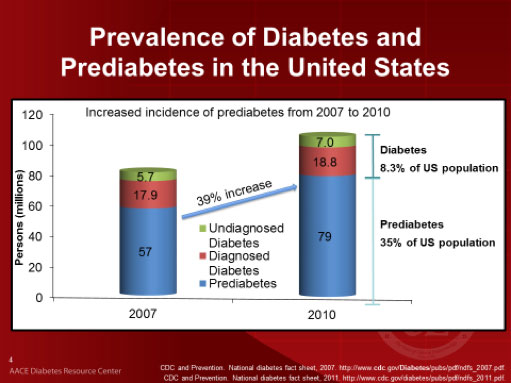
How common is prediabetes (insulin-resistance)? Take a look at Figures 3 and 4.
According to the research cited above, the incidence of prediabetes rose 39% from 2007 to 2010. Prediabetes and Type 2 diabetes are curable conditions.
According to the CDC, without lifestyle changes to improve their health, 15% to 30% of people with prediabetes will develop Type 2 diabetes within five years. What are the risk factors for prediabetes? They include:
- Age, especially after 45
- Being overweight or obese
- A family history of diabetes
- Having an African American, Hispanic/Latino, American Indian, Asian American, or Pacific Islander racial or ethnic background
- A history of diabetes while pregnant (gestational diabetes) or having given birth to a baby weighing nine pounds or more
- Being physically active less than three times a week
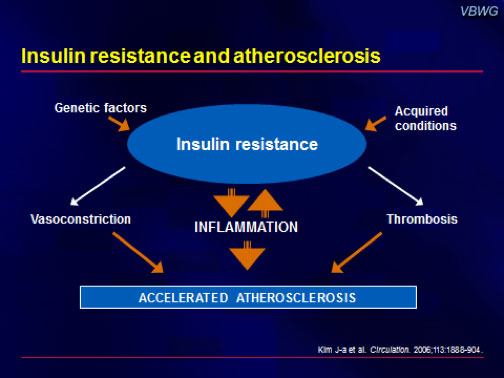
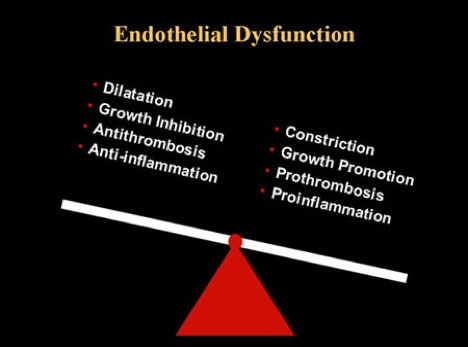
Figure 5 notes some of the causes and symptoms of insulin-resistance, while Figure 6 focuses on the connection between insulin-resistance and atherosclerosis.
Insulin-resistance occurs prior to Type 2 diabetes, but still increases the risk of thrombosis (blood clot), hypertension (high blood pressure), inflammation and heart disease.
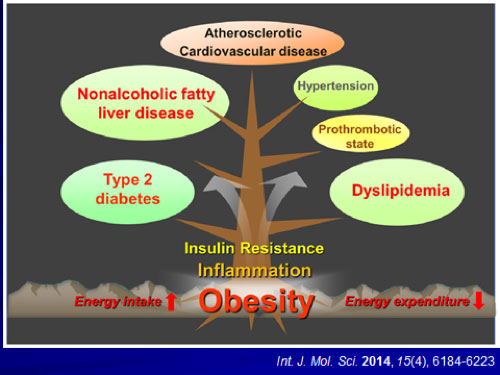
As noted in Figure 7, obesity — especially abdominal obesity — is one of the predominant underlying risk factors for insulin-resistance. Obesity increases the risk of developing a variety of pathological conditions, including insulin-resistance, Type 2 diabetes, dyslipidemia (abnormal cholesterol), hypertension (high blood pressure) and NAFLD (non-alcoholic fatty liver disease). Accumulating evidence suggests that chronic inflammation in adipose tissue may play a critical role in the development of obesity-related metabolic dysfunction.
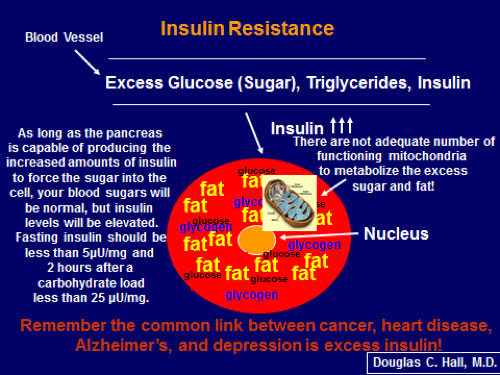
As documented in Figure 8, the common link between heart disease, cancer, Alzheimer’s and depression is excess insulin, not excess glucose. Alzheimer’s is now called Type 3 diabetes.
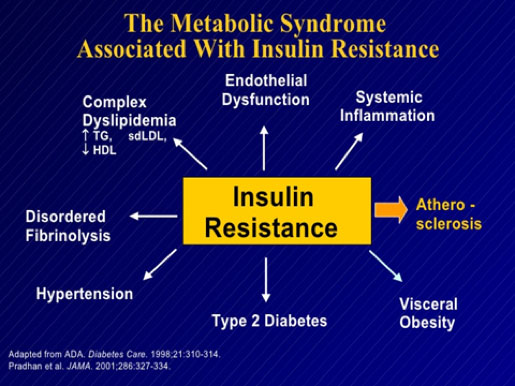
The conditions that are associated with insulin-resistance are noted in Figures 9 and 10.